Services

Cancer Diagnosis
India faces a huge burden of cancer, very often diagnosed in the late stages. Such delayed detection compromises patient outcomes. Hence, in the fight against cancer, early and accurate diagnosis is of paramount importance. It represents the first step in creating an effective treatment plan.
Diagnosis usually begins with a thorough medical history, physical examination, and a review of symptoms. Depending on the case, doctors may recommend imaging tests such as X-rays, CT scans, MRIs, or PET scans to look for abnormal growths or tumors.
In addition, laboratory tests on blood, urine, or other body fluids can provide important information, which can be correlated with other findings. A biopsy, where a small tissue sample is taken and examined under a microscope, remains the most reliable way to confirm cancer. Advances in molecular and genetic testing now allow doctors to understand the specific type and behaviour of a tumor, helping in customizing treatment plans best suited for each patient. This approach is referred to as personalized medicine.
It is natural to feel anxious when facing a diagnosis, but patients should remember that it is the foundation for effective care. Open communication with the oncologist is important to clarify doubts and understand results. Seeking a second opinion can also provide reassurance and confidence in the recommended approach.

Chemotherapy
Chemotherapy is a powerful drug therapy designed to target and destroy rapidly growing cells in the body, making it a common treatment for cancer. It serves two main purposes: treating cancer by curing it, reducing the likelihood of recurrence, or slowing its growth, and easing cancer symptoms by shrinking tumors that cause pain or other complications. 2 Often, chemotherapy is combined with other treatments like surgery, radiation, or hormone therapy, depending on factors such as the cancer’s stage and type, your overall health, previous treatments, and personal preferences.
As a systemic treatment, chemotherapy affects the entire body. It is typically administered in cycles, consisting of a treatment phase followed by a rest period to allow the body to recover and produce new healthy cells. For example, a cycle might involve daily treatment for one week followed by three weeks of rest, forming a four-week cycle. Chemotherapy has been a reliable cancer treatment for decades, either eliminating cancer or improving quality of life by reducing symptoms.
Targeted Therapy
Targeted therapy is a specialized cancer treatment that focuses on genetic changes or mutations that turn healthy cells into cancer cells. To determine the right treatment, healthcare providers first test for the genetic changes that enable cancer cells to grow and survive. Unlike traditional therapies, targeted therapy disrupts specific processes cancer cells rely on, such as blocking signals for blood vessel growth (angiogenesis inhibitors), interfering with protein digestion within cancer cells (proteasome inhibitors), and disrupting the messaging systems cancer cells use to multiply (signal transduction inhibitors).
Targeted therapies use small-molecule drugs or antibodies to attack specific cancer cell targets. They enhance the immune response, block cancer growth, or deliver toxins directly to the cells. This treatment is effective for various cancers, including blood cancers, lung cancers, breast cancers, digestive system cancers, and reproductive system cancers (prostate, cervical). Targeted therapy can stop cancer cells from growing, block the blood supply to tumours, or help the immune system fight cancer better. It also allows for delivering treatments like chemotherapy directly to cancer cells, reducing damage to healthy tissue. This precision approach makes targeted therapy a promising option for managing and treating specific cancer types.
Immunotherapy
Immunotherapy is a cancer treatment that helps the body's immune system to fight cancer. While the immune system can prevent or slow cancer growth, cancer cells often find ways to evade detection or destruction. They may alter their genetic makeup to become less visible to the immune system, produce proteins that turn off immune responses, or modify surrounding normal cells to interfere with immune activity. Immunotherapy works by enhancing the immune system's ability to recognize and attack cancer cells, making it an essential treatment for certain types of cancer.
Immunotherapy uses our immune system to fight cancer and can be used alone or in combination with other cancer treatments, depending on factors like the type and stage of cancer, as well as previous treatments. There are several types of immunotherapies, including monoclonal antibodies (MABs), checkpoint inhibitors, vaccines, cytokines, and CAR T-cell therapy. This treatment is particularly beneficial for cancers that have not responded to traditional treatments or have returned after treatment, offering hope for more effective outcomes in challenging cases.
Radiation Therapy
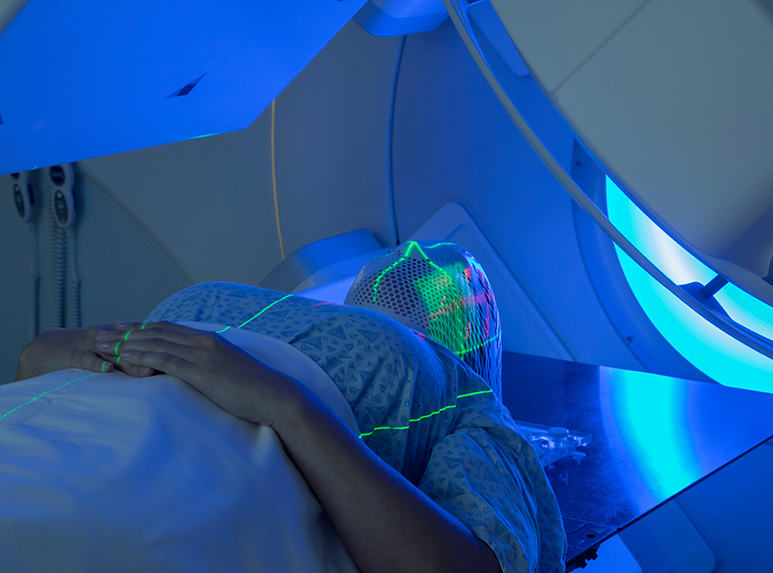
Radiation therapy, also known as radiotherapy, is a common cancer treatment that uses high-energy radiation, typically X-rays to destroy cancer cells by damaging their DNA. Without intact DNA, cancer cells lose the ability to grow and divide, leading to tumor shrinkage.
Radiation therapy may be the only treatment for some, but it's often combined with surgery, chemotherapy, or immunotherapy. It can be given before, during, or after other treatments to improve outcomes. The timing depends on the cancer type and whether the goal is to treat the cancer or relieve symptoms.
Radiation therapy can shrink tumors before surgery (neo-adjuvant), eliminate residual cancer cells after surgery (adjuvant), or treat recurring cancers. It is also used to relieve cancer-related symptoms and may even help treat noncancerous tumors causing discomfort. Beyond cure, radiation plays a key role in palliative care—helping ease symptoms and improving quality of life, so patients can live more comfortably and meaningfully.
Onco Surgery
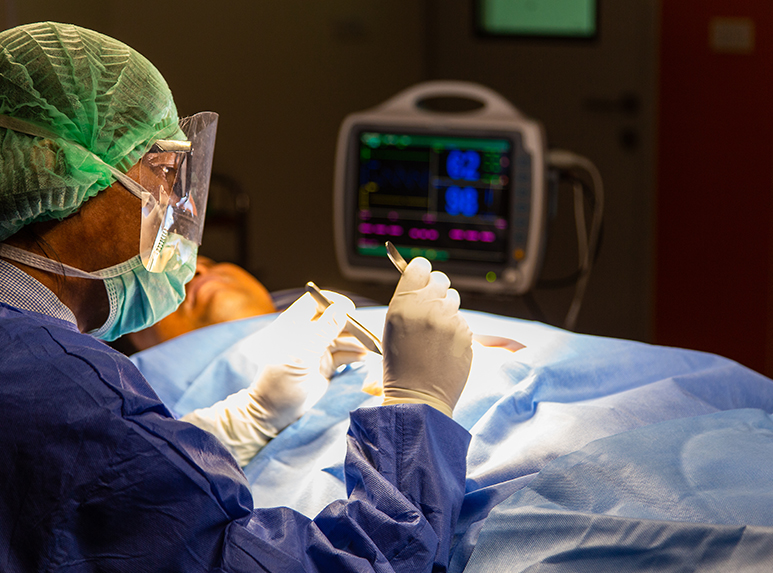
Cancer surgery is a key part of cancer care, often used for diagnosis, treatment, and even prevention. In some cases, surgery can remove an organ or tissue before cancer develops, helping lower the risk of certain cancers. It also plays a role in diagnosis by providing tissue samples for testing, which can confirm cancer and guide personalized treatment plans. Surgery may be used to determine the cancer’s stage, serve as the main treatment, or reduce tumor size when complete removal isn’t possible. Additionally, it can relieve symptoms like pain or blockages caused by tumors. Often combined with chemotherapy or radiation, cancer surgery is tailored based on cancer type, stage, and the patient’s overall health, making it a vital component in comprehensive cancer treatment.
Cancer surgery is typically performed with the goal of removing the entire tumor along with a margin of healthy tissue to ensure no cancer cells remain. Surgeons may also remove nearby lymph nodes to check for signs of cancer spread, which helps guide further treatment.
Whether surgery is an option depends on several factors, such as the type and location of the cancer, its stage, and the patient’s overall health. Surgery is generally most effective for solid tumors and may not be suitable for cancers that originate in the blood or lymphatic system.

Palliative care
Palliative care is specialized medical care focused on relieving pain, managing symptoms, and improving the quality of life for individuals with serious illnesses and their families. Early integration can reduce depression, anxiety, and enhance satisfaction with care, sometimes even extending survival. It supports various conditions, including cancer, heart and lung diseases, kidney failure, dementia, HIV/AIDS, etc. Delivered by a team of healthcare specialists, palliative care ensures comfort, dignity, and holistic support throughout the illness.
Palliative care addresses the multifaceted impact of serious illness. For physical challenges like pain, shortness of breath, or nausea, the care team may offer medications, physical therapy, or nutritional guidance. Emotional and social difficulties, including anxiety, depression, or caregiver stress, are managed through counselling, support groups, and mental health referrals. Practical concerns such as financial or legal issues are addressed by connecting families with resources and guidance. Additionally, spiritual care is available to help patients and families explore beliefs and find peace. 2 Studies show that early palliative care not only enhances quality of life but can also extend survival, reduce anxiety, and improve overall satisfaction with care.
Cancer Treatment
The choice of treatment depends on the type of cancer, its stage, and the patient’s overall health. Common approaches include surgery, chemotherapy, radiation therapy, targeted therapy, and immunotherapy. Often, a combination of these treatments is used to achieve the best results. Surgery may be recommended to remove tumors, while chemotherapy and radiation work to destroy cancer cells or shrink tumors before surgery.
In the era of genetic testing of cancers, personalized medicine approaches, with treatment plans tailored to maximize efficacy in every case, are being frequently employed in cancer care. Such advances in precision medicine now allow treatments to be tailored to the genetic profile of an individual’s cancer, leading to improved outcomes with fewer side effects. Targeted therapies are designed to block specific molecules that cancer cells need for their survival, while immunotherapy helps the body’s own immune system recognize and attack cancer more effectively. In some cases, hormonal therapy or stem cell transplantation may also be used.
Supportive care, such as pain management, nutritional support, and counselling, also plays a crucial role in helping patients maintain quality of life during treatment. Each patient’s journey is unique, and treatment plans are made collaboratively between the oncologist and patient. With timely intervention and modern therapies, many cancers can be controlled, treated effectively, or even cured.
CAR-T Cell therapy
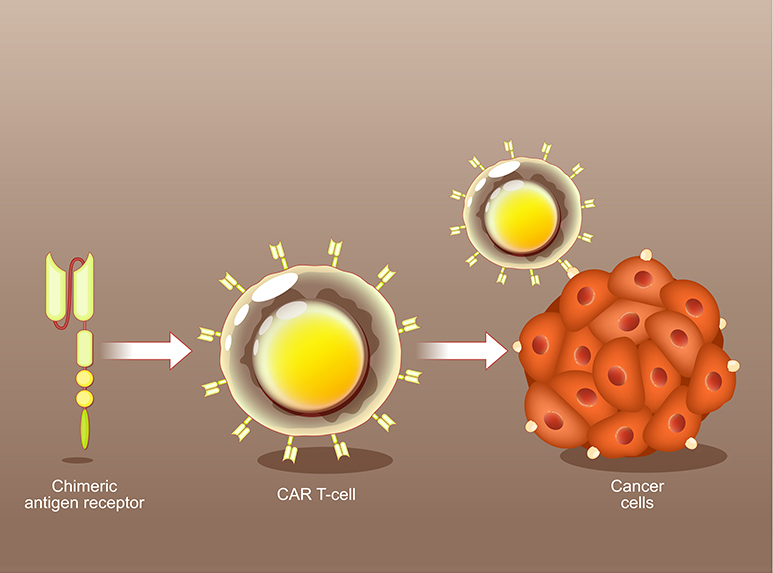
Chimeric Antigen Receptor (CAR) T-cell therapy is an innovative immunotherapy designed to combat certain blood cancers. It works by changing your T cells (a type of immune cell) to better find and destroy cancer cells. This makes them more effective at fighting cancer.
Before receiving CAR T-cell therapy, patients may need treatments like chemotherapy or radiation to control cancer while the CAR T-cells are being prepared. A week before the therapy, a special type of chemotherapy called lymphodepletion is done to reduce existing T cells and prepare the body for the therapy. The CAR T-cells are then infused through an IV, similar to a blood transfusion, which takes about 5 to 30 minutes.
After the infusion, patients usually stay in the hospital for 7 to 10 days to monitor for side effects, followed by close observation for the first month. CAR T-cell therapy offers hope for patients who don’t respond to other treatments or have recurring cancer. Studies show that over 85% of children with acute lymphoblastic leukemia achieve remission (cancer treatment reduces or eliminates the symptoms and signs of cancer), with 60%, remaining cancer-free a year later.
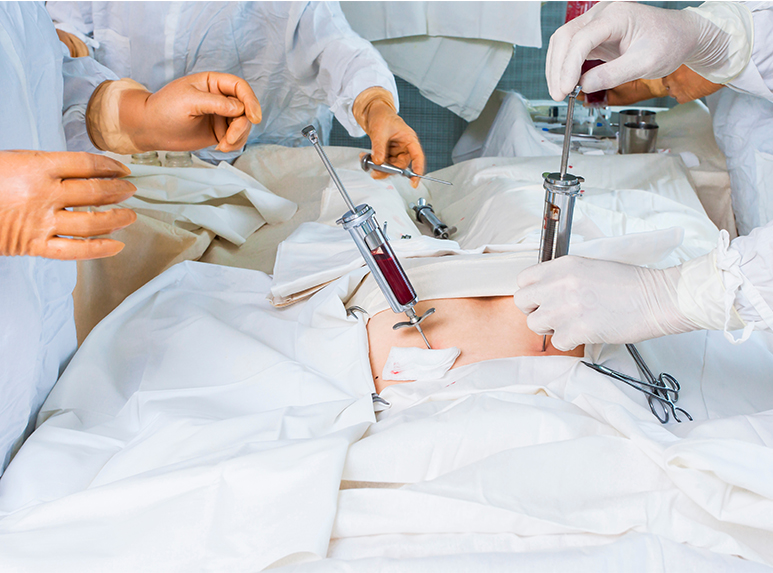
Bone marrow transplant
Pain management
Cancer pain can range from mild to severe and may take various forms, such as sharp, stabbing pain that comes and goes, tingling or burning sensations, or a persistent ache. It significantly impacts quality of life, potentially worsening cancer symptoms, treatment side effects, and increasing the risk of depression and anxiety.
Effective pain management for cancer often involves medications tailored to the patient's needs. Non-opioid pain relievers like acetaminophen, ibuprofen, and naproxen are typically used for mild to moderate pain and are available over the counter. For more severe pain, opioids like morphine, fentanyl, and oxycodone are prescribed, often in combination with other treatments. Additionally, other medications, including anticonvulsants, antidepressants, or steroids, may be recommended for specific pain types, such as nerve pain or pain due to inflammation. Finding the right medicine and dosage may take time, but healthcare providers aim to minimize side effects while effectively controlling pain.
Beyond medications, several alternative treatments can help manage cancer pain. These include nerve blocks, which involve injecting anesthetics to block pain signals, and nerve stimulation techniques like TENS, which use mild electrical currents to alleviate discomfort. In rare cases, surgical procedures like cordotomy may be performed to sever specific nerves near the spinal cord. Alternative therapies such as acupuncture, hypnosis, and relaxation techniques can complement standard treatments, offering additional relief and improving overall well-being.

Counselling
Cancer can take a toll not just on the body but also on a person’s emotional well-being, often affecting daily life, relationships, and future plans. The shock of a cancer diagnosis can be overwhelming, making it harder to cope with everyday challenges.
Cancer counselling offers crucial mental health support, helping patients process their emotions, manage anxiety, and navigate difficult thoughts. Counsellors provide a safe space to express feelings, untangle worries, and find clarity, while guiding individuals toward acceptance and personal solutions. This emotional support plays a vital role in helping patients face cancer with resilience and strength.
Trained counsellors help individuals navigate the emotional impact of cancer through talk therapy, allowing them to express their true feelings and learn healthy coping strategies. While counselling does not treat the disease itself, it can ease the mental burden and empower patients and caregivers alike to face the journey ahead with greater clarity, confidence, and emotional resilience.
There are different types of therapy that support emotional well-being during cancer care. Behavioural therapies help manage negative thoughts and behaviours, while psychoanalytical and psychodynamic therapies explore deep-rooted patterns formed in childhood. Humanistic therapies focus on the present moment, encouraging self-awareness and personal growth to cope better with the current challenges.
